In the media, it is often the “case fatality rate” that is talked about when the risk of death from COVID-19 is discussed.1
This measure is sometimes also called case fatality risk or case fatality ratio. It is often abbreviated as CFR.
The CFR is not the same as the risk of death for an infected person – even though, unfortunately, journalists sometimes suggest that it is. It is relevant and important, but far from the whole story.
The CFR is easy to calculate. You take the number of people who have died from the disease, and you divide it by the total number of people diagnosed with the disease. So if 10 people have died, and 100 people have been diagnosed with the disease, the CFR is [10 / 100], or 10%.
But it’s important to note that it is the ratio between the number of confirmed deaths from the disease and the number of confirmed cases, not total cases. That means that it is not the same as – and, in fast-moving situations like COVID-19, probably not even very close to – the true risk for an infected person.
Another important metric, which should not be confused with the CFR, is the crude mortality rate.
The “crude mortality rate” is another very simple measure which, like the CFR, gives something that might sound like the answer to the question “if someone is infected, how likely are they to die?”.
But, just as with CFR, it is actually very different.
The crude mortality rate – sometimes also called the crude death rate – measures the share among the entire population that have died from a particular disease. It’s calculated by dividing the number of deaths from the disease by the total population. For instance, if there were 10 deaths in a population of 1,000, the crude mortality rate would be [10 / 1,000], or 1%.
Unfortunately, writers sometimes confuse case fatality rates and crude death rates. A common example is the Spanish flu pandemic in 1918. One estimate for the death toll of the Spanish flu, by Johnson and Mueller (2002), is that the pandemic killed 50 million people.2 That would have been 2.7% of the world population at the time. This means the crude mortality rate was 2.7%.
But 2.7% is often misreported as the case fatality rate – which is wrong, because not everyone in the world was infected with the virus that caused the Spanish flu. If the crude mortality rate really was 2.7%, then the case fatality rate was much higher – it would be the percentage of people who died after being diagnosed with the disease. [We looked at the global death count of the Spanish flu pandemic and others here.]
The key question for understanding the mortality risk of a disease is the following: if someone is infected with the disease how likely is it that they will die from it? The answer to that question is captured by the infection fatality rate, or IFR.
The IFR is the number of deaths from a disease divided by the total number of cases. If 10 people die of the disease, and 500 actually have it, then the IFR is [10 / 500], or 2%.3,4,5,6,7
To work out the IFR, we need two numbers: the total number of cases and the total number of deaths from the disease.
However, as we explain here, the total number of cases of COVID-19 is not known. One big reason for this is that not everyone with COVID-19 is tested.8,9
The total number of cases is not known, so the IFR cannot be simply calculated from observed data. But, researchers are able to estimate the total number of cases and use that to calculate the IFR – we get to this further below.
There is a straightforward question that most people would like answered. If someone is infected with COVID-19, how likely is that person to die?
This question is simple, but surprisingly hard to answer.
The key point is that the case fatality rate (CFR) – the most commonly discussed measure – is not the answer to the question.
The main reason why it does not answer that question is that the CFR relies on the number of confirmed cases, and many cases are not confirmed.
In order to understand what the case fatality rate can and cannot tell us about a disease outbreak such as COVID-19, it’s important to understand why it is difficult to measure and interpret the numbers.
Sometimes commentators talk about the CFR as if it’s a single, steady number: an unchanging fact about the disease.
But it’s not a biological constant; instead, it reflects the situation in a particular context, at a particular time, in a particular population.
The probability that someone dies from a disease doesn’t just depend on the disease itself, but also on the treatment they receive, and on the patient’s own ability to recover from it.
This means that the CFR can decrease or increase over time, as responses change; and it can vary by location and by the characteristics of the infected population, such as age, or sex. For instance, older populations would expect to see a higher CFR from COVID-19 than younger ones.
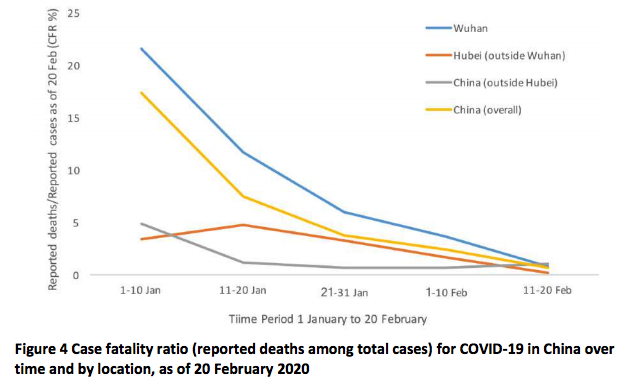
The case fatality rate of COVID-19 is not constant. This was clear right from the start of the pandemic. You can see that in the chart below, first published in the Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-19), in February 2020.10
It shows the CFR for COVID-19 in several locations in China during the early stages of the outbreak, from the beginning of January to 20th February 2020.
You can see that in the earliest stages of the outbreak the CFR was much higher: 17.3% across China as a whole (in yellow) and greater than 20% in the center of the outbreak, in Wuhan (in blue).
But in the weeks that followed, the CFR declined, reaching as low as 0.7% for patients who first showed symptoms after February 1st. The WHO reported that that was because “the standard of care has evolved over the course of the outbreak”.
You can also see that the CFR was different in different places. By 1st February, the CFR in Wuhan was still 5.8% while it was 0.7% across the rest of China.
This shows that what we said about the CFR generally – that it changes from time to time and place to place – is true for the CFR of COVID-19 specifically. When we talk about the CFR of a disease, we need to talk about it in a specific time and place – the CFR in Wuhan on 23rd February, or in Italy on 4th March – rather than as a single unchanging value.
Case fatality ratio for COVID-19 in China over time and by location, as of 20 February 2020 – Figure 4 in WHO (2020)11
If the case fatality rate does not tell us the risk of death for someone infected with the disease, what does it tell us? And how does the CFR compare with the actual mortality risk?
There are two reasons why we would expect the CFR not to represent the real risk. One of them would tend to make the CFR an overestimate – the other would tend to make it an underestimate.
When there are people who have the disease but are not diagnosed, the CFR will overestimate the true risk of death. With COVID-19, we think there are many undiagnosed people.
As we saw above, in our discussion on the difference between total and confirmed cases (here), we do not know the number of total cases. Not everyone is tested for COVID-19, so the total number of cases is higher than the number of confirmed cases.
Whenever there are cases of the disease that are not counted, the probability of dying from the disease is lower than the reported case fatality rate. Remember our imaginary scenario with 10 deaths and 100 cases. The CFR in that example is 10% – but if there actually 500 cases (and we’ve simply missed 400 of them due to lack of testing), then the real risk (the IFR) is just 2%.
Or to summarize in one sentence. If the number of total cases is higher than the number of confirmed cases, then the ratio between deaths and total cases is smaller than the ratio between deaths and confirmed cases.12
Importantly, this means that the number of tests carried out affects the CFR – you can only confirm a case by testing a patient. So when we compare the CFR between different countries, the differences do not only reflect rates of mortality, but also differences in the scale of testing efforts.
A second consideration is especially important in the early stages of an outbreak: When some people are currently sick and will die of the disease, but have not died yet, the CFR will underestimate the true risk of death.
In ongoing outbreaks, people who are currently sick will eventually die from the disease. This means that they are currently counted as a case, but will only eventually be counted as a death too. With the COVID-19 outbreak, it can take several weeks for people to go from first symptoms to death.
This means that the CFR in the early stages is an underestimate of what it will be when the outbreak has run its course.
What we do know if that the mortality risk is higher for older populations and those with underlying health conditions such as cardiovascular disease, diabetes and respiratory disease – we look at some preliminary evidence for this in our full coverage of the COVID-19 pandemic here.